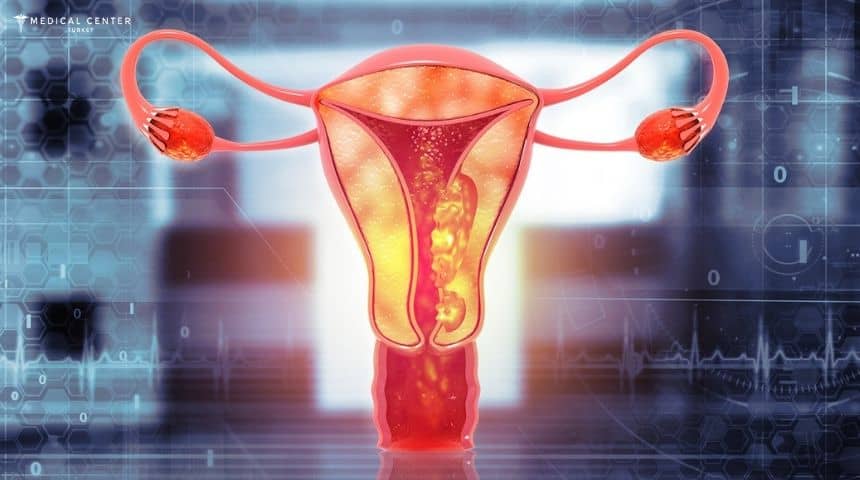
Uterine Cancer in Turkey
Uterine Cancer in Turkey is an article that aims to give you all the information you do not know about uterine cancer and more. We kindly shared the main headings with you;
What is uterine cancer?
A general term used to describe cancer of the uterus is uterine cancer. The endometrium, or inner lining of your uterus, is where endometrial cancer begins to grow. This is among the most prevalent gynecologic cancers or cancers of the reproductive system. The uterine muscle wall, or myometrium, is where uterine sarcomas grow. Rarely do uterine sarcomas occur.
What is the function of uterus and endometrium in Turkey?
The reproductive system of women and individuals assigned female at birth includes the uterus (AFAB). Pregnancy occurs in the uterus, where a fetus grows and develops. The term body or corpus refers to the upper portion of the uterus. The cervix, which connects the uterus to the vagina, is located at the lower end of the uterus. Cancer of the uterus is referred to as uterine cancer, while cervical cancer is a distinct type of cancer that affects the cervix. Both conditions are medically evaluated and treated in Turkey by specialized gynecological oncology units.
The inner lining of the uterus is called the endometrium. Throughout the menstrual cycle, the endometrium undergoes regular changes. When pregnancy occurs, the endometrium thickens under the influence of the hormones progesterone and estrogen to support fetal development. When the body does not produce enough progesterone for pregnancy, the endometrial lining sheds, resulting in menstruation. These physiological processes and related health conditions are routinely monitored and managed in Turkey within women’s healthcare services.
What are the risk factors of uterine cancer?
Among the risk factors are:
- Age. The probability of having uterine cancer rises with age. After age 50, uterine malignancies typically manifest.
- High animal fat diet. Eating a diet heavy in fat can raise your risk of developing multiple malignancies, including uterine cancer. Additionally rich in calories are fatty foods, which can contribute to obesity.
- Diabetes. Obesity is a risk factor for cancer and is frequently linked to this disease. However, other research points to a closer connection between diabetes and uterine cancer.
- Being obese (being overweight). Certain hormones are converted to estrogen by adipose tissue, which increases the risk of uterine cancer. The influence on estrogen levels increases with the amount of fat tissue present.
- Ovarian diseases. Individuals with specific ovarian cancers have low progesterone and excessive estrogen levels. These hormonal variations may raise the risk of uterine cancer.
- Family history. Hereditary diseases that raise the risk of cancer can be inherited by some persons. Individuals who have Lynch syndrome, also known as hereditary nonpolyposis colorectal cancer (HNPCC), are more likely to develop endometrial cancer in addition to other cancers.
What are the symptoms of uterine cancer?
Uterine cancer symptoms might mimic those of a variety of illnesses. This is particularly true for various disorders affecting the reproductive system. See your doctor in Turkey if you experience any unusual pain or erratic vaginal bleeding. Obtaining a precise diagnosis is essential to receiving the appropriate care. Endometrial cancer and uterine sarcoma symptoms include:
- Vaginal bleeding before menopause in between cycles
- A small amount of vaginal bleeding or spotting following menopause
- Cramping or lower abdominal pain in the area of your pelvis directly beneath your belly
- If you are postmenopausal, you may have thin, clear, or white vaginal discharge
- Severe, persistent, heavy, or frequent vaginal bleeding in women over 40
What is the diagnosis of uterine cancer?
To confirm a uterine cancer diagnosis, your doctor may run one or more tests:
Blood examinations
The CA-125 assay quantifies the protein CA-125. Your body may be showing signs of cancer if your CA-125 level is elevated.
Imaging examinations
For imaging examinations CT scan, MRI scan, and transvaginal ultrasound is used.
- CT scan produces several finely detailed images of your internal organs.
- A strong magnet and radio waves are used in MRI scans to produce images.
- A smooth, spherical device called a transvaginal ultrasonography probe is inserted into your vagina to take images of your uterus.
Additional examinations
Additional examinations include endometrial biopsy, hysteroscopy, and D&C.
- A thin, flexible tube is inserted during an endometrial biopsy procedure via the cervix, the opening of the uterus, and into the uterus. Your doctor takes off a tiny portion of the endometrium.
- During a hysteroscopy, a long, thin tube called a hysteroscope is inserted into your cervix and vagina to reach your uterus. This slender device with a light camera captures fine-grained pictures of your uterus.
- The more involved technique of dilation and curettage (D&C) is used to remove uterine tissue. Your clinician then sends the sample to a lab if you had a D&C or biopsy to remove tissue samples. A pathologist examines the tissue there to see whether cancer is present.
What is the staging of uterine cancer?
The cancer stage will also be determined by your physician. On a scale from I to IV, uterine cancers are categorized.
- Stage I: You only have stage I cancer in your uterus.
- Stage II: The cancer is stage II and has reached your cervix.
- Stage III: The ovaries, lymph nodes, and/or vagina have all been affected by stage III cancer.
- Stage IV: Cancer has progressed to distant organs from your uterus, such as your bladder. In certain situations, your doctor might not be able to identify the stage of your cancer until after you’ve had surgery to remove it.
- In addition to determining the stage, treatment costs are closely related to the stage of uterine cancer. In earlier stages, such as Stage I or II, treatment is often more limited and may involve surgery alone or combined with short-term therapy, which generally results in lower overall costs. However, in advanced stages like Stage III and IV, treatment becomes more complex and prolonged, often requiring a combination of surgery, chemotherapy, radiation therapy, and extended follow-up care. These additional procedures and longer treatment durations significantly increase the total cost of care. Therefore, early diagnosis and staging not only influence treatment options but also play a critical role in managing the overall financial burden of uterine cancer treatment.
You can easily request a personalized treatment plan and receive your free quote by clicking the image below.
What are the treatment types of uterine cancer?
Surgery
The main course of treatment for endometrial cancer is typically surgery. The surgeon will probably perform a hysterectomy on you, during which your uterus and cervix will be removed. Hysterectomy techniques come in four different varieties:
- Complete abdominal hysterectomy: To access and remove your uterus, the surgeon creates a cut in your abdomen. During a vaginal hysterectomy, your uterus is removed by the surgeon through your vagina.
- Radical hysterectomy: You might require a radical hysterectomy if cancer has progressed to your cervix. Your uterus and the tissues around it are removed by the surgeon. Along with the cervix, the surgeon also removes the upper portion of the vagina. In a minimally invasive hysterectomy, your uterus is removed by the surgeon through several tiny incisions. Either robotics or laparoscopy can be used for this.
In addition to a hysterectomy, surgeons frequently carry out the following two procedures:
- Bilateral salpingo-oophorectomy (BSO): Both your fallopian tubes and ovaries will be removed during a bilateral salpingo-oophorectomy (BSO). To ensure that all cancer is removed, the majority of patients require this extra step.
- Lymph node dissection: Lymph node dissection, or lymphadenectomy, to remove nodes and check for the spread of malignancy.
The side effects of uterine cancer may include fertility, and the inability to conceive. Menopause includes associated symptoms, such as vaginal dryness and night sweats (if you were premenopausal and had your ovaries removed) are other possible side effects.
Other treatment types
The majority of endometrial cancer patients require surgery. The specific course of treatment for you will depend on the type of cancer and your general health. Other therapies you might receive consist of:
- Chemotherapy, which kills cancer cells by administering potent medications.
- Radiation therapy, which utilizes tailored radiation beams to kill cancer cells.
- Hormone therapy, which treats cancer by either blocking or supplying hormones. Immunotherapy, which is an aid to the immune system in the battle against cancer.
- Targeted therapy, which involves the use of drugs to target particular cancer cells and prevent them from proliferating.
How to take care of yourself after the treatment?
After your treatment is completed, your healthcare team in Turkey will discuss your follow-up care plan with you in detail. Attending follow-up visits is essential, as these appointments help ensure long-term recovery and early detection of any potential recurrence. During a follow-up visit in Turkey, your healthcare provider will typically perform a pelvic examination and ask about any symptoms you may be experiencing.
The primary goals of follow-up care are to monitor your overall health, detect any signs of cancer recurrence, and support your physical and emotional well-being after treatment. These visits also provide an opportunity to discuss healthy lifestyle strategies with your healthcare professional in Turkey.
Adopting habits such as regular exercise, balanced nutrition, and adequate sleep can help you feel your best and improve your quality of life after cancer treatment. Comprehensive follow-up care in Turkey plays a vital role in supporting recovery and maintaining long-term health.
Why choose Turkey for uterine cancer?
Several factors influence the decision to receive treatment for uterine cancer in Turkey, therefore it’s important to take individual circumstances, preferences, and medical needs into account. Turkey is becoming more and more known as a destination for medical tourism because it provides cutting-edge medical facilities, highly qualified medical personnel, and a rich cultural experience. For the treatment of uterine cancer, people may think of traveling to Turkey for the following reasons:
- Advanced Healthcare Establishments: Turkey boasts contemporary, well-equipped medical facilities because of large investments in its healthcare infrastructure. Modern technology is commonly used at leading hospitals for postoperative care, diagnosis, and treatment.
- Skilled Healthcare Practitioners: Turkish medical personnel with substantial training and experience include gynecologic surgeons, oncologists, and support personnel. Many graduate from prestigious international medical schools.
- Economical Medical Care: Turkish medical care is frequently less expensive than in other Western nations, which attracts people looking for high-quality care without the exorbitant price tag.
- Superior Quality Cancer Care: Turkey is renowned for offering top-notch cancer therapies, such as radiation therapy, chemotherapy, surgery, and other cutting-edge treatments. Most of the time, the therapies comply with international standards.
- Privacy and Confidentiality: Turkish medical facilities frequently place a high value on patient privacy and confidentiality, offering cancer patients a safe and encouraging environment.
To decide on the best course of action, people should do extensive research, ask for advice, and speak with their healthcare experts before making any decisions. To guarantee a thorough grasp of the diagnosis and treatment alternatives, it is crucial to confirm the qualifications of healthcare professionals and institutions, comprehend the available treatment options, and get a second opinion.
If you want to consult a medical professional try our free consultation service. Medical Center Turkey is always here to help you.