How Long is Bone Marrow Transplant?
How Long is Bone Marrow Transplant? is an article that aims to give you all the information you do not know about how long is a bone marrow transplant and more. We kindly shared the main headings with you;
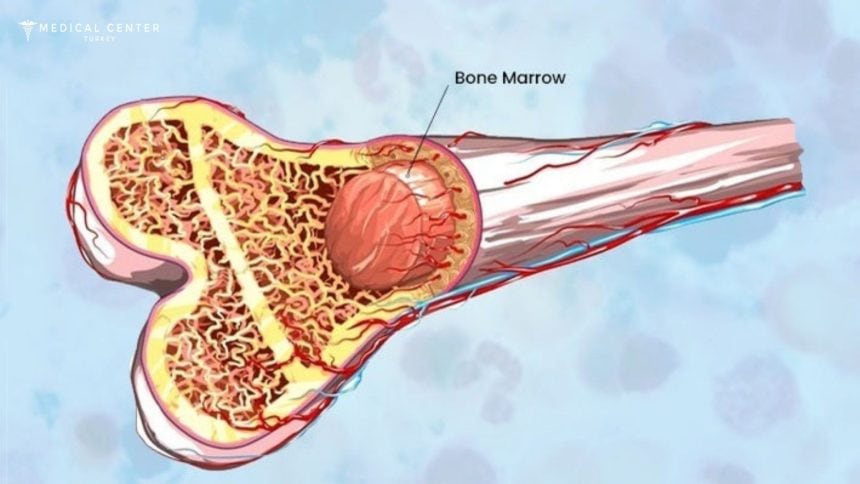
What is a bone marrow?
The interior of the bones contains a spongy material called bone marrow. It creates materials like bone marrow stem cells, which in turn create blood cells. Each type of blood cell produced by the bone marrow serves a crucial function. Oxygen is delivered to human tissues via red blood cells. Through aiding blood clotting, platelets reduce bleeding. Viruses are fought by white blood cells.
What is a bone marrow transplant?
In order to replace bone marrow that isn’t creating enough healthy blood cells, a bone marrow transplant injects your body with healthy blood-forming stem cells. Another name for a bone marrow transplant is a stem cell transplant. If your bone marrow stops producing enough healthy blood cells or stops functioning altogether, you may require a bone marrow transplant. Both autologous (using your own cells) and allogeneic (using donor cells) types of bone marrow transplants are possible.
What are the reasons to get a bone marrow transplant?
A bone marrow transplant can be used to:
- Replace or repair the bone marrow that has been harmed by the treatment in order to safely tolerate large doses of chemotherapy or radiation.
- Replace malfunctioning bone marrow with fresh stem cells.
- Provide fresh stem cells that can directly combat cancer cells.
Invest in your health, invest in a brighter future. Our comprehensive medical programs deliver real results, while you indulge in the beauty and serenity of our destination.
Who can benefit from bone marrow transplant?
Many malignant and non-cancerous diseases, such as the following, can be treated by bone marrow transplants:
- Acute leukemia
- Adrenoleukodystrophy
- Aplastic anemia
- Bone marrow failure syndromes
- Chronic leukemia
- Hemoglobinopathies
- Hodgkin’s lymphoma
- Immune deficiencies
- Inborn errors of metabolism
- Multiple myeloma
- Myelodysplastic syndromes
- Neuroblastoma
- Non-Hodgkin’s lymphoma
- Plasma cell disorders
- POEMS syndrome
- Primary amyloidosis
What are the types of bone marrow transplant?
There are two types of bone marrow transplant which are Allogeneic stem cell transplant and Autologous stem cell transplant.
Allogeneic Stem Cell Transplant
In an allogeneic stem cell transplant, healthy blood stem cells from a donor are used to replace bone marrow that is not producing enough healthy blood cells. An alternative term for an allogeneic stem cell transplant is an allogeneic bone marrow transplant. A donor could be a close friend, a family member, or even a complete stranger. Blood stem cells can include the following in an allogeneic stem cell transplant:
- Drawn from the blood of the donor
- Taken out of the donor’s hipbone’s bone marrow
- Derived from umbilical cord blood that had been donated
![]()
![]()
A patient receiving an allogeneic stem cell transplant will
- Receive cancer treatment (conditioning) at high doses. You will receive heavy doses of chemotherapy or radiation therapy during the conditioning process to eradicate your cancer cells. Your sickness and unique circumstances will determine the course of your treatment. The conditioning process’s cancer treatments run the danger of having negative side effects. Discuss the expected outcomes of your treatment with your doctor.
- Receiving a stem cell infusion. Your blood will be infused with donor stem cells, which will then move to your bone marrow and start the process of producing new blood cells.
- Being under careful medical supervision. Your medical team will want to closely watch you for any issues after your transplant. You might stay there or in the neighborhood for a few weeks. Blood tests and consultations to check on your progress after the transplant should be expected frequently.
The donor cells must settle in your bone marrow for a few weeks before they can start producing new cells. Blood transfusions may be necessary as your bone marrow heals.
Autologous Stem Cell Transplant
An autologous stem cell transplant replaces damaged bone marrow with healthy blood stem cells from your body. An autologous bone marrow transplant is another name for an autologous stem cell transplant. When compared to stem cells from a donor, using your own cells for a stem cell transplant has several benefits. For instance, if you receive an autologous stem cell transplant, you won’t need to be concerned about the compatibility of the donor’s cells with your own cells.
If enough healthy bone marrow cells are being produced by your body, an autologous stem cell transplant may be an option. It is possible to gather, freeze, and preserve such cells for later use. An autologous stem cell transplant entails:
- Using drugs that will boost your blood’s stem cell level. You’ll be given medicines that make your stem cells more numerous and travel from your bone marrow into your blood, where it’s easier to harvest them.
- Filtering blood stem cells for analysis. A needle is used to draw blood from a vein in your arm in order to obtain stem cells. The remaining blood is returned to your body after the stem cells are removed by a machine. Your stem cells are given a preservative before being frozen and kept for future use.
- Receiving cancer treatment (conditioning) at high doses. Receiving a stem cell infusion. After being injected into your bloodstream, your stem cells will move to your bone marrow and start the process of producing new blood cells.
![]()
![]()
How to get prepared for the surgery?
There are three main components for the preparation stage. These include,
Tests and procedures
Your general health and the condition of your condition can be evaluated using a number of procedures and tests. You are physically prepared for the transplant thanks to the examinations and treatments as well. The evaluation could go on for a few days or longer. In addition, an intravenous catheter will be inserted into a large vein in your neck or chest. The catheter, also known as a central line, usually stays in place throughout the course of your treatment. The central line will be used by the transplant team to inject your body with the transplanted stem cells, medicines, and blood components.
The conditioning process
You will start a process called conditioning after finishing the pretransplant exams and procedures. During conditioning, you will receive chemotherapy and perhaps radiation treatment to
- If you are being treated for cancer that could spread to other parts of your body, eliminate malignant cells
- Suppress your immune system
- Get your bone marrow ready to receive the new stem cells.
Your overall health, the ailment you are treating, and the sort of transplant you are getting will all influence the type of conditioning procedure you get. As part of your conditioning treatment, you might have radiation in addition to chemotherapy, or only one of these therapies alone.
Several side effects are,
- Nausea and vomiting
- Diarrhea
- Hair loss
- Mouth sores or ulcers
- Infection
- Bleeding
- Infertility or sterility
- Anemia
- Fatigue
- Cataracts
- Organ complications, such as heart, liver or lung failure
Reduced-intensity conditioning
You might receive lesser doses or different kinds of radiation or chemotherapy as part of your conditioning treatment, depending on your age and medical history. Reduced-intensity conditioning is what is meant by this. Reduced-intensity conditioning weakens your immune system while killing some cancer cells. After that, your body receives the donor’s cells via infusion. Over time, cells in your bone marrow are replaced by donor cells. The donor cells’ immune components may then battle your cancer cells.
What to expect from bone marrow transplant surgery?
Before the procedure
High doses of chemotherapy or radiation therapy, or perhaps both, will be administered to you during the conditioning process in an effort to eradicate your cancer cells. This process is called conditioning. The treatments you receive are determined by your disease and unique circumstances. The conditioning process’s cancer treatments run the danger of having negative side effects. Discuss the expected outcomes of your treatment with your doctor.
During the procedure
It takes one to two hours to complete the transplant procedure. Healthy cells from your donor will be taken out by an IV (intravenous) catheter (again, similar to giving blood) and then transfused into you through a central line to get your new bone marrow cells. This process is painless. You won’t be put to sleep and will be fully alert. The new healthy cells enter your bone marrow through a procedure called engraftment, where they multiply to eventually take control and develop a healthy marrow and immune system.
![]()
![]()
You finish the conditioning procedure before your bone marrow transplant. Stem cells are administered into your body through your central line on the day of your transplant. The infusion for the transplant is painless. Throughout the procedure, you will be awake.
After the procedure
Your blood carries new stem cells to your bone marrow after they have entered your body. They gradually grow in number and start to produce fresh, healthy blood cells. It’s known as engraftment. Before your body’s blood cell count starts to return to normal, it often takes a few weeks. It could take longer in certain individuals.
You’ll get blood tests and other examinations to check on your health in the days and weeks following your bone marrow transplant. To treat issues including nausea and diarrhea, you may need medication. Following your bone marrow transplant, you’ll continue to receive close healthcare.
You can anticipate spending 30 to 60 days in the hospital or at the outpatient clinic for your transplant, while every patient’s circumstances are different depending on the kind of transplant and the likelihood of problems. You might need to stay in the hospital for a few days or longer if you have infections or other issues. Until your bone marrow starts making enough red blood cells and platelets on its own, you might also require recurring transfusions of those blood components.
What to pay attention to in recovery period?
After your transplant, it’s even more crucial to take cancer prevention measures. Be sure to pay attention to the followings,
- Medications. Your immune system needs time to heal after a transplant. You may be given antibiotics during this period.
- Check-ups. For months or years following your transplant, you could be more susceptible to infections or other problems. You will continue to visit your doctor regularly for the rest of your life to look for any potential issues. Make sure to receive the recommended cancer screenings to see the progress of your treatment.
- Diet. You might need to change your diet after your bone marrow transplant to keep healthy and avoid gaining too much weight. Additionally, your dietician might recommend foods to help you manage nausea caused by chemotherapy and radiation side effects. Your dietitian might advise observing food safety recommendations that can help prevent foodborne diseases, consuming fruits, vegetables, whole grains, lean meats, poultry, fish, legumes, and healthy fats like olive oil, consuming less salt, and avoiding grapefruit and grapefruit juice because it interacts with immunosuppressive drugs.
- Physical activity. Following your bone marrow transplant, frequent physical exercise aids in weight management, bone and muscle health, increased endurance, and heart health. As you heal, you may gradually increase your physical activity.
- Avoid smoking.
- Use sunscreen. When you’re outside, wear sunscreen.
What are the risks of getting a bone marrow transplant?
Numerous dangers can result from a bone marrow transplant. While some recipients of a bone marrow transplant have minor issues, others may develop severe problems that necessitate medical attention or hospitalization. Life-threatening consequences can occasionally occur. The sickness or condition that necessitated the transplant, the type of transplant, your age, and your general health all affect your risks.
Following a bone marrow transplant, problems could arise, including:
- Graft-versus-host disease (a complication of allogeneic transplant only)
- Stem cell (graft) failure
- Organ damage
- Infections
- Cataracts
- Infertility
- New cancers
Your medical professional can describe the potential risks associated with a bone marrow transplant. In order to determine whether a bone marrow transplant is the best option for you, you can analyze the risks and advantages together.
What is Graft-versus-host disease?
You may be at risk of graft-versus-host disease (GVHD) if you have an allogeneic transplant, which involves stem cells from a donor. This disorder develops when your body’s tissues and organs are attacked by donor stem cells that make up your new immune system. GVHD might occur any time after your transplant. GVHD is a common side effect of allogeneic transplantation. If the stem cells are from an unrelated donor, there is a higher risk of developing GVHD. But everyone who receives a bone marrow transplant from a donor can develop GVHD.
Acute and chronic GVHD are the two different types. Acute GVHD typically develops in the first few months following your transplant. Usually, it has an impact on your liver, digestive system, or skin. Chronic GVHD can affect several organs and often manifests later in life.
The signs and symptoms include:
- Joint or muscle pain
- Shortness of breath
- Persistent cough
- Vision changes, such as dry eyes
- Skin changes, including scarring under the skin or skin stiffness
- Rash
- Yellowing of the skin and the whites of your eyes
- Dry mouth
- Mouth sores
- Diarrhea
- Nausea
- Vomiting
You may take medications to help prevent graft-versus-host disease (GVHD) and lessen your immune system’s reactivity if your bone marrow transplant uses donor stem cells (allogeneic transplant). These medicines are referred to as immunosuppressive drugs.
What is life expectancy after the surgery?
With more precise genetic matching between recipients and donors, transplantation followed by an antibiotic regimen to manage infections, and enhanced post-transplant care generally, the life expectancy, survival rate, and quality of life following a bone marrow transplant have all significantly improved.
What is the cost of a bone marrow transplant?
The overall cost of a stem cell transplant varies significantly depending on the type of treatment and the patient’s specific medical needs. Several medical and logistical factors play a role in determining the total cost, making each treatment plan highly individualized.
Key factors affecting the cost include the type of stem cell transplant performed, the complexity of the procedure, and whether the stem cells are sourced from the patient or a donor. Additional medical treatments, such as chemotherapy, pre-transplant conditioning, hospitalization, medications, and supportive therapies, can substantially influence the total treatment cost.
Post-transplant care is another important cost component. Follow-up visits, laboratory tests, ongoing monitoring, and medications required during the recovery period are essential for treatment success and may affect the overall cost.
For patients traveling from abroad, non-medical expenses should also be considered. These may include travel arrangements, accommodation, local transportation, and daily living expenses during the treatment and recovery period. In some cases, donor-related procedures and collection processes may also contribute to the total cost.
Because of these variables, stem cell transplant costs are best determined through a personalized medical evaluation. A detailed treatment plan provides a transparent breakdown of included services, allowing patients to understand what is covered and to plan their treatment more effectively.
You can easily request a personalized treatment plan and receive your free quote by clicking the image below.
Does insurance cover for the bone marrow transplant surgery?
The price of a stem cell transplant mostly relies on each patient’s insurance coverage. Insurance coverage could pay all or part of the cost of the operation. Furthermore, a lot of organizations and resources provide financial aid and other support services to help with the cost of medical treatment associated with a stem cell transplant. Make careful to fully investigate each choice before deciding which one is best for your circumstances.